Ths peer reviewed article was first published in the journal Tuith OnlineGeneral dental practitioners view on the pursuit and practice of evidence-based dentistry: The results of a questionnaire.This is a full version of this report. If you would like, read the summary report. This survey into the views of trainers and trainees in general dental practice was carried out as a pilot study. It was conducted amongst two particular groups of dentists, and the findings are not presented as being necessarily representative of the opinions or otherwise of the approximately 2,800 dentists practising in Scotland. This survey, though small, has given a good insight into the some of the barriers standing in the way of a more complete adoption of evidence-based practice into dental primary care and highlighted differences and similarities between the understanding or perceived understanding of two groups at different stages of their careers. IntroductionThe practice of evidence-based medicine, including evidence-based dentistry, is a process of life-long, problem-based learning in which caring for patients can be aided by knowledge of disease processes, prognosis, therapy, and other clinical and healthcare issues. There are also ethical and legal requirements for practitioners to provide effective evidence-based treatment, rather than outdated, experimental, or otherwise less effective non-evidence-based treatment (Cannavina et al 2000). At the end of 1998, there were 29,951 dentists registered with the General Dental Council (including 2,810 with addresses in Scotland) the majority of whom work within the National Health Service to provide clinical care (General Dental Council 1999). Thus the bulk of the expenditure and clinical activity is undertaken by general dental practitioners (GDP), however, the majority of research into clinical dentistry is undertaken by dental schools with some investigations being undertaken within the community dental service. The findings of this research activity are presented primarily in peer reviewed journals in a format which busy GDPs can find unhelpful and, possibly, confusing. In addition to the academic journals, healthcare providers, researchers, and policy makers are inundated with unmanageable amounts of information from other sources. To address such problems, systematic reviews (Mulrow 1994) and meta-analysis (Oxman 1993; Sacks 1987; L'Abbe 1987; Thacker 1988) attempt to establish where the effects of healthcare choices are consistent and which research results may be usefully applied across different populations and settings; thus aiding decisions between differences in treatment (NHS CRD 1999). This survey was undertaken to ascertain to what extent trainers and trainees in general dental practice embraced the conclusions of dental research, how they attempted to incorporate new conclusions on best practice into their day to day treatment strategies, how much difficulty they experienced in keeping up to date in their practice, and whether they believed, in any case, that research findings had anything to offer them and their patients. Subjects and MethodsThe survey questionnaires were handed out on two separate occasions to target two distinct populations of primary care dentists; the first being persons responsible for providing vocational training and the second those undergoing training. Each group was attending a one day courses on critical appraisal and the opportunity was thus presented to compare the attitudes of these two groups of dentists towards the issues examined in this report. For the purposes of the survey, respondents were provided with a definition for evidence-based dentistry based on a published definition for evidence-based medicine (Sackett et al. 1996): "the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients. Its practice means integrating individual clinical expertise with the best available external clinical evidence from systematic research." They were then posed a series of questions where they were invited to grade their opinions on a non-numerical, arbitrary scale, between strong disagreement with the sentiment of the question and strong agreement, by placing a cross on a horizontal line. Further questions were asked concerning the respondents opinions on the best way to move towards evidence-based practice, what the major barriers were to this, how much use they made of the various sources of guidance in existence, and to what extent respondents were able to understand the specialist terms used in academic literature. Results43 questionnaires were completed in total, 24 by the trainer group and 19 by the trainee group, though some respondents did not answer all questions. Attitudes towards evidence-based dentistry The replies of the respondents to the questions concerning their attitude towards
the value and practice of evidence-based dentistry are shown in figure
1. Figure 1 Respondents attitudes towards evidence-based dentistry (lanes 1-6: 0 to 5, positive attitude; 0 to -5, negative attitude; lane 7 is percentage. Light blue boxes represent trainees) 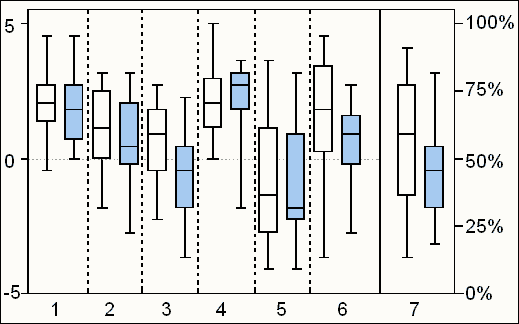
Questions
There was good agreement between the two surveys, carried out between the two groups of dentists, but with mean scores being lower for the trainees on 6 out of the 7 questions. Statistically, there was no difference between the two groups at the 95% confidence level, apart from question 3 on the usefulness of research in day to day management of patients which was border line. When asked which was the most appropriate route to move from opinion-based
practice towards evidence-based dentistry and given a choice of: a) identifying
and appraising the primary literature or systematic reviews themselves,
b) seeking and applying evidence-based summaries which give the clinical
bottom line, c) or using evidence-based practice guidelines developed
by others, 54.2% (13/24) of the trainers and 47.4% (9/19) of the trainees
favoured the latter option. Only 16.7% (4/24) and 21.1% (4/19), respectively,
thought it was appropriate that they should appraise the literature themselves
(figure 2) and almost the same proportion said they were, in fact, doing
so. In contrast, 41.7% of the trainers and an enthusiastic 63.2% of the
trainees thought that they might be interested in following this route
at some time in the future. 45.8% (11/24) of the trainers (compared to
only 15.8% (3/19) of the trainees, said they were using evidence-based
summaries but, despite this disparity, apparently similar numbers, 29.2%
(7/24) and 31.6% (6/19) respectively, thought that these were an appropriate
aid to practice. Figure 2 Moving from opinon-based to evidence-based practice. Which route is most appropriate? 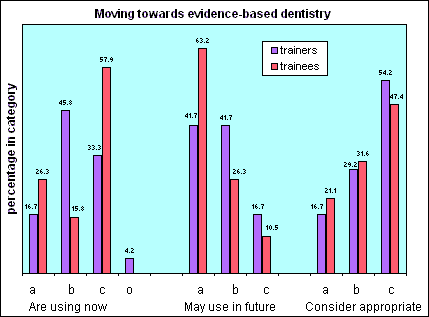
Key:
Accessing the evidence Amongst the trainer group, the majority of respondents (18/24) had not recently used a bibliographic database such as Medline for literature searching. Of those who had, the topics of interest were infectious prophylaxis for endocarditis, periodontics, oral medicine, dental pain, Bell's Palsy, adhesive dentistry, and Hepatitis C. Only 1 in 8 (3/24) had received training in literature searching strategies. 41.6% (10/24) reported formal training in critical appraisal and 17.4% (4/23) had attended other related courses, for example as part of vocational training. Although only 6 respondents had recently used Medline, 11 (45.8%) said they had access at home, 2 (8.3%) in their surgeries, and 5 (20.8%) in a local medical library. Greater numbers had access to the World Wide Web (on which free access to Medline is available from PubMed or BioMedNet) with 19 (79.2%) having access at home, 6 (25%) in the surgery, and 8 (33.3%) at a local medical library. In complete contrast to the above, 17 of the 19 trainees said that they had used Medline or similar within the last year, with frequencies varying between slight use and regular use. The topics showed some overlap with, but also differences from, the other group and included endodontics, periodontics, oral cancer, mouthguards, toothwear, and composite - glass ionomer comparisons. Access to Medline, and the world wide web, was for this group chiefly at a University library: not surprising as most would be living in temporary lodgings. A third (7/19) had received formal training in information searching and most (15/19) in critical appraisal, but only one person had attended another course (apart from the one being attended when the questionnaire was handed out) in evidence-based dentistry. Amongst the trainers, there was a relatively low awareness of review publications and relevant databases with only 25% (6/24) reporting having read the journal "Evidence-Based Dentistry" and half this number (3/24) having consulted the "Effective Health Care Bulletins". Only 2 trainees had read the first of these and none the second. Within both groups, there were two people only who said they had used information from these two publications as a basis for a clinical decision and some of the named sources were completely unknown to most respondents. When asked to list other sources of useful information, postgraduate courses, clinical research associates, dental journals, and the Dentanet web-site were mentioned. Facilitating the practice of evidence-based dentistry. When asked "How could the practice of evidence-based dentistry be further facilitated in your own practice?", suggestions included; activities involving discussion between all members of the dental team, including journal clubs and other literature reviewing activities, backed up by clinical audit, payment of fees for attending courses and for adopting new protocols, and concise, reader friendly guidelines. This latter point was highlighted by a number of respondents who felt that more attention needs to be given to pre-filtering information and advice offered to busy practitioners in advance of the production of better produced and more soundly based protocols and guidelines. The major barriers to practising EBD were perceived to be mainly those of time and resources. Respondents felt that GDPs needed more training to acquire new skills and encouragement to change 'old habits'. They suggested that literature was inaccessible to many of them and much of the evidence of poor quality and badly presented. It was also felt that ethical issues, patients' views, and need for consistency were other areas that needed to be addressed to further improvements in the quality of care for patients. Understanding technical terms in the literature. GDPs cannot be expected to
judge the value of research publications if they are unable to understand
the technical terms used, which are often intended to convey a precise
meaning. When asked to quantify their understanding of certain terms,
it is apparent that there is a range of comprehension, from terms such
as meta-analysis and odds ratio, of which there is virtually no understanding,
to terms such as publication bias, number needed to treat, and clinical
effectiveness which a majority of respondents amongst the trainers felt
confident that they had a good understanding of (figure 3). 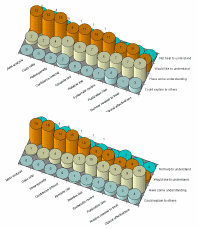
Click on image to view larger size Between these two extremes, there proved to be a mixture of levels of comprehension but, overall, very few respondents had a great deal of confidence in their understanding of any of the listed terms: certainly not enough to explain their use to others. The trainers and the trainees were quite similar in their estimations of their abilities and knowledge. One item where they did apparently differ was that only 16.6% (4/24) of trainers had some or good understanding of confidence intervals compared to a self-estimated 47.4% (9/19) of those being trained. DiscussionEvidence-based treatment requires that the professionals involved are up to date in their knowledge of current understandings on best practice and that they have, or are willing and able to acquire, the appropriate skills and competencies. It has been estimated that, at the current time, only a limited number of dental health procedures fulfil the strict criteria of EBP, most being based on much less rigorous criteria (Cannavina, 2000). This survey has revealed that amongst the groups questioned, individuals were welcoming towards the idea of EBD but differed in their enthusiasm and, if their estimates are accurate, differed even more strikingly in the proportion of their current practice which was evidence-based, from a low of less than 14% to an upper estimate of more than 90%. Although respondents agreed that EBP led to an improvement in patient care it is surprising that at the same time there appeared to be a belief that EBD, in general, is of limited value because primary care lacks a scientific grounding. The survey queried whether respondents were likely to, or thought it appropriate that they should, access evidence themselves from primary sources. The most appropriate route for moving from opinion-based to evidence-based practice supported by just over half the respondents (22/43) was using guidelines and protocols developed by others. Despite this, the results showed a predicted move away from use of pre-digested guidelines towards self appraisal (figure 2). Most of the trainee dentists said they had consulted sources such as Medline within the year prior to the question being posed, however, a majority of the respondents from the trainer group had not recently consulted bibliographic databases and most of both groups were unaware of many of the review publications and extracting journals available. Some of those dentists in the trainer group, who had consulted such sources, may have done so to seek information to help with a particular condition which had occurred recently in their practice: some examples were given. The trainees may have consulted them as part of their studies. Many of the terms employed in technical reports are of a specialist nature and are often used to convey a narrow meaning which is not intuitive and may even be counter-intuitive. Certain words and terms may be familiar to readers, but can be used to convey specialist meanings which might not be obvious unless specifically defined. Non-specialists reading such terms often do not grasp the full significance of what they are reading and this is a barrier to understanding which was confirmed by the answers given in this questionnaire. For example, only one person had 'some understanding' of meta-analysis and three of odds ratio. Thus it is not surprising that respondents were keen for interpretation and summary of the specialist literature to be carried out by people with the necessary background. Of other barriers identified, popular ones were lack of time and resources. It was suggested that the fee structure could be used to encourage take up of new techniques and attendance on suitable courses. Some respondents were keen to involve all members of the dental team, to get together to review procedures and the literature, and to take account of the patients' perspective and views. ConclusionThis survey, though small, has given a good insight into the some of the barriers standing in the way of a more complete adoption of evidence-based practice into primary care dentistry and highlighted differences and similarities between the understanding or perceived understanding of two groups at different stages of their careers. The major barriers are perceived to be mainly those of time and resources. It was felt that more attention should be given to the pre-processing of information, that is reducing long, expansive papers into short, focused reports. This was because busy dentists could not afford to devote time to extracting information from academic literature. However, there was relatively little knowledge of review publications and this may indicate that such publications may not be reaching this audience. Training, without loss of income, was highlighted as the way to acquire new skills and change 'old habits'. This survey has acted as a pilot study. It was conducted amongst two particular groups of dentists, and the findings are not presented as being necessarily representative of the opinions or otherwise of the approximately 2,800 dentists practising in Scotland. The pilot study will be followed up with a much larger survey of about 500 Scottish dentists drawn at random from Scotland Dentists. ReferencesGeneral Dental Council. The Dentists Register 1999. London GDC 1999. Cannavina, C.D., Cannavina, G., and Walsh, T.F. (2000) Effects of evidence-based treatment and consent on professional autonomy. British Dental Journal 188: 302-306. Mulrow, C.D. (1994) Rationale for systematic reviews. British Medical Journal 309: 597-599. Oxman, A.D. (1993) Meta-statistics: Help or hindrance? ACP Journal Club 118: A-13. Sacks, H.S., Berrier, J., Reitman, D., Ancona-Berk, V.A., and Chalmers, T.C. (1987) Meta-analysis or randomised controlled trials. New England Journal of Medicine 316: 450-455. L'Abbe, K.A., Detsky, A.S., and O'Rourke, K. (1987) Meta-analysis in clinical research. Annals International Medicine 107: 224-233. Thacker, S.B. (1988) Meta-analysis: a quantitative approach to research integration. Journal of the American Medical Association 259: 1685-1689. NHS Centre for Reviews and Dissemination. (1999) Database of abstracts of reviews of effectiveness. In: Cochrane Library, Issue 2. Update Software, updated quarterly. Reviewers:
Authors
|
|
Web space provided by the University of Dundee,
maintained by
the Dental Health Services Research Unit. Valid XHTML1.0
|
 |
Evidence-based dentistry web-site | |